HEMS provide prehospital critical care on behalf of the statutory ambulance service in the East of England (The East of England Ambulance Service NHS Trust (EEAST)) to a population of over six million people over a geographic area of 20,000 km 2, dispatched by either rotary wing (H145 (EAAA), AW169 (EHAAT/Magpas), or MD902 (EHAAT)) or rapid response vehicle, depending on patient location, weather constraints, and time of day. 
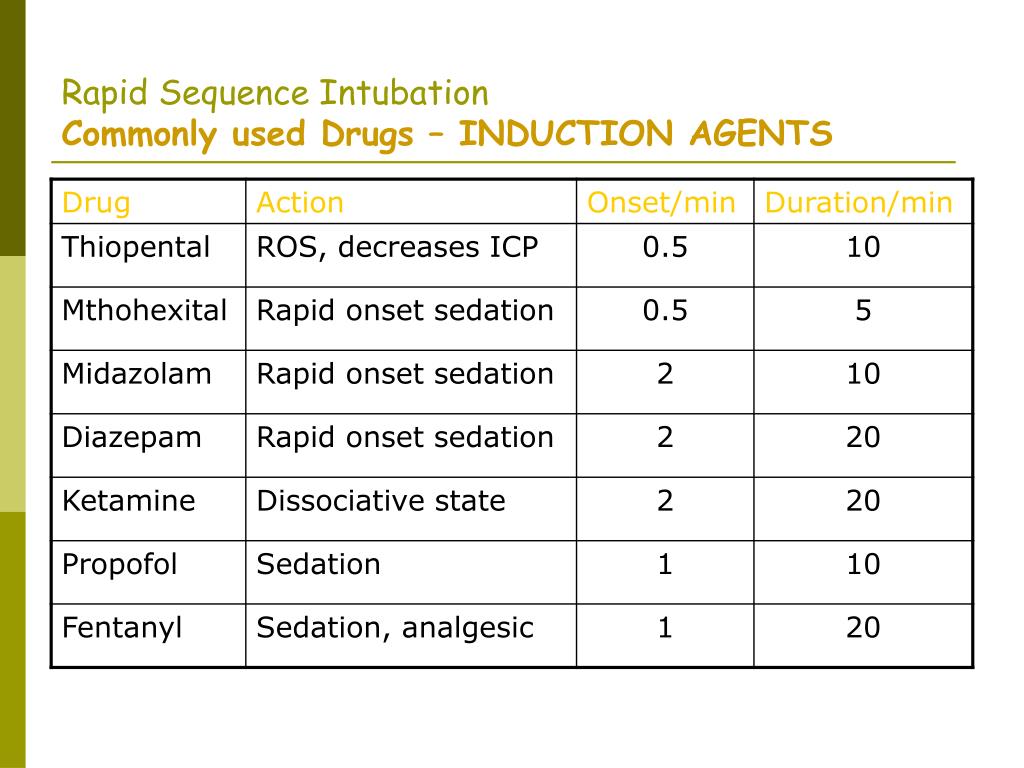
The study was performed in three UK HEMS with five operational bases: two are operated by East Anglian Air Ambulance (EAAA), two by Essex & Herts Air Ambulance (EHAAT), and one by Magpas Air Ambulance (Magpas). The objective of this multi-centre observational study was to compare the differential determinants of PIH in a large cohort of undifferentiated adult trauma patients. Previous publications on this topic include small sample sizes with an inherent inability to reliably characterise the determinants of PIH. The factors associated with PIH in critically injured patients are not well understood but are likely to be a combination of haemorrhage, cardiac depression from contusions and/or hypoxia, negative inotropy and vasoplegia from anaesthetic agents, acidaemia secondary to hypercapnia during peri-intubation apnoea, and reduced venous return from positive-pressure ventilation. Therefore, prehospital key performance indicators include the incidence of PIH as a marker of quality in UK HEMS practice. PIH after PHEA is prevalent, and is associated with increased mortality in trauma. These protocols yield favourable intubating conditions, but the addition of an opioid may increase the risk of post-intubation hypotension (PIH). The historical use of etomidate and suxamethonium has been superseded by fentanyl, ketamine, and rocuronium administered either in a full dose (3:2:1) or reduced dose (1:1:1) regime. Simple, standardised RSI protocols are recommended for PHEA to promote reproducible techniques and reduce human error. ĭrug-assisted rapid sequence induction (RSI) is used to facilitate prehospital emergency intubation. 
UK Helicopter Emergency Medical Services (HEMS) deliver prehospital emergency anaesthesia (PHEA) more than two-thousand times per year, predominantly in patients with traumatic head injury, where meticulous avoidance of hypoxia and hypotension are key to reducing secondary brain injury and improving outcomes. In the United Kingdom (UK), a significant proportion of the most seriously injured trauma patients have airway compromise requiring intervention that exceeds the capabilities of the statutory ambulance service. Clinician gestalt and provider intuition is likely to be the strongest predictor of PIH, suggested by the choice of a reduced dose induction and/or the omission of fentanyl during the anaesthetic for patients perceived to be at highest risk. The variables significantly associated with PIH only account for a small proportion of the observed outcome. Induction drug regimes in which fentanyl was omitted (0:1:1 and 0:0:1 (rocuronium-only)) were the determinants with the largest effect sizes associated with hypotension. Hypotension was defined as a new systolic blood pressure (SBP) 10% reduction if SBP was 55 years old pre-PHEA tachycardia multi-system injuries and intravenous crystalloid administration before arrival of the HEMS team were the variables significantly associated with PIH. Consecutive sampling of trauma patients who underwent PHEA using a fentanyl, ketamine, rocuronium drug regime were included, 2015–2020. This multi-centre retrospective observational study was performed across three Helicopter Emergency Medical Services (HEMS) in the UK. The objective of this study was to compare the differential determinants of PIH in adult trauma patients undergoing PHEA. Post-intubation hypotension (PIH) after prehospital emergency anaesthesia (PHEA) is prevalent and associated with increased mortality in trauma patients.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
